Breast Reconstruction Surgery
About Breast Reconstruction Surgery
The decision to reconstruct the breast after a mastectomy may not be an easy one, and the many choices available for reconstruction will likely only add to the confusion. At Farkas Plastic Surgery, we are committed to doing everything possible to help guide you through the many choices and decisions that you will face. We know you are going through a very difficult time, and it is our goal to make the process as seamless as possible for you. Please feel free at any time to contact Dr. Farkas or any member of the staff directly with any questions or concerns that you may have.
Explore Topics On This Page:
A Diagnosis of Breast Cancer
A diagnosis of breast cancer unfortunately is extraordinarily common and is a traumatic event for every woman and family. For many of these women, treatment with breast conservation surgery (i.e. lumpectomy) may be an option. For others however, treatment with mastectomy may be the recommendation from the breast surgeons. All questions related to your breast cancer care are best suited for your excellent breast cancer team and surgeons. For those who undergo mastectomy, losing a breast can have a devastating psychological impact in one’s self-image and self-confidence, however with the revolutionary breast reconstructive techniques of plastic surgery the older disfiguring cancer surgery is a thing of the past. Novel plastic surgical breast reconstruction now has the ability to provide women with a natural appearing breast shape following their mastectomy. As recent as 25 years ago, options for post-mastectomy breast reconstruction were severely limited. Furthermore, the results of those procedures in use were generally unnatural and lacking. Fortunately, advances in plastic surgery made since that time have enabled us to offer both single and double mastectomy patients several excellent options for breast reconstruction.
Procedures for Breast Reconstruction
The main advantage of autologous breast reconstruction is that because the breast is reconstructed with the patient’s own tissues, it is the most “natural” reconstruction as these tissues will heal and grow with the patient, and require no maintenance or upkeep.
The main disadvantage of autologous breast reconstruction techniques are the donor site changes, which in some cases can be advantageous like when taken from the abdomen or medial thigh.
In recent years, there have been dramatic technical advances in autologous breast reconstruction, which is considered by many to be the “gold standard” of breast reconstruction. Advances in microvascular surgery, such as the DIEP flap have made it possible to transfer the necessary tissue with minimal trauma to the donor site. This has resulted in dramatically reduced donor site problems without compromising the outcome of the breast reconstruction. Furthermore, these technological advances have made the option of autologous breast reconstruction a reality for patients who previously were not considered good candidates.
However, infrequent issues, such as pseudo-hernias (aka abdominal bulge), fat necrosis, partial flap losses, numbness, and weakness may be a long standing complication of autologous reconstruction. Furthermore, autologous breast reconstructions surgical procedures generally take slightly longer than other implant based options on account of the technical aspect of the surgery. Lastly and most importantly, unfortunately not every patient is a candidate for an autologous breast reconstruction. Factors such as body habitus, previous surgeries, smoking history, and co-exsiting medical conditions may be prohibitive. Dr. Farkas will discuss all of this information with you in great detail at your in office consultation. The autologous reconstruction can either be performed at the time of the mastectomy or depending on the need for post mastectomy radiation in a “delayed” fashion. If post mastectomy radiation is planned, then usually a tissue expander would be placed at the time of the mastectomy and act as a spacer until the autologous reconstruction is performed. It is generally delayed six months after the completion of the radiation therapy to allow for adequate healing to the soft tissues and chest.
The second excellent option for breast reconstruction, is an implant based breast reconstruction. This technique uses breast implants, either silicone or saline, to reconstruct the breast mound. This can be performed as either a single stage (permanent implant placed same time as the mastectomy) or two stage procedure (using an expander followed by implant insertion) depending on your breast size and shape. The tissue expander or implant can be placed either above the pectoral muscle (pre-pectoral) or under the muscle (submusclar).
Dr. Farkas will discuss the benefits and disadvantages of each of these types of reconstruction in detail. Prosthetic breast reconstruction techniques spare the patient the loss of donor site tissue as well as donor site scarring. It is currently recommended by the FDA to have the implants evaluated for possible exchange 10-15 yrs after placement. If a tissue expander if placed, the patient will have weekly expansions that usually begin two weeks following the mastectomy until the desired volume is achieved. Once the volume of the expanded pocket is deemed adequate the soft tissue heals for approximately 4-6 weeks and then the permanent implant is exchanged at a second operation.
The third option for breast reconstruction uses a combination of the first two options. This option involves the transfer of the patients own tissues (usually from the back or abdomen) in combination with the insertion of a tissue expander or implant. This option encompasses both the advantages and disadvantages of autologous and prosthetic breast reconstruction techniques. It is generally used when an implant reconstruction is planned but there is a lack of healthy, pliable soft tissue at the mastectomy site or insufficient donor soft tissue volume. For patients undergoing mastectomy for breast cancer, health insurance will generally cover a portion of the procedure cost. Although Farkas Plastic Surgery is Out of Network with all insurance company’s and managed care plans (except Medicare), we do accept most types of insurance payments and as a courtesy to our patients, we will submit the precertification and claims directly to the insurance company on our patients’ behalf. In some cases there could be out of pocket expenses relative to your insurance plan.
Deep Inferior Epigastric Artery Perforator Flap (DIEP)
The deep inferior epigastric artery perforator flap is a newer abdominally based reconstruction option for select patients that over the past 15 years has supplanted the free transverse rectus abdominal muscle (TRAM) flap. The DIEP flap uses the abdominal skin and fat only avoiding the sacrifice of the rectus abdominus muscles (6-pack muscles) improving the post-operative recovery, with less pain, and preventing any future abdominal wall weakness.
The procedure is very similar to the free TRAM flap with disconnecting the arteries and veins in the groin and reconnecting them microscopically to an artery and vein in the chest. However, the arteries and veins are dissected free from the rectus abdominus muscle leaving it in place un- injured are sacrificed.
Post operatively there is an incision along the inferior portion of the abdomen from hip to hip and around the belly button similar to the scars of an abdominoplasty (tummy tuck). Depending on the type of mastectomy that was performed the incisions on the breast are generally the same incisions used to place the flap in the chest.
Patients who have had prior abdominal surgeries may still be candidates for the reconstruction and we get a pre-operative MRA of the abdomen to use as a map of the blood vessels of the abdomen to ensure that there is adequate vascular supply for the flap procedure.
Post-operatively patients are monitored in the intensive care unit for flap monitoring purposes only for 24-48 hrs and usually have a 3-5 day hospital stay.
Deep Inferior Epigastric Artery Perforator Flap (DIEP)
Pedicled TRAM Flap Breast Reconstruction
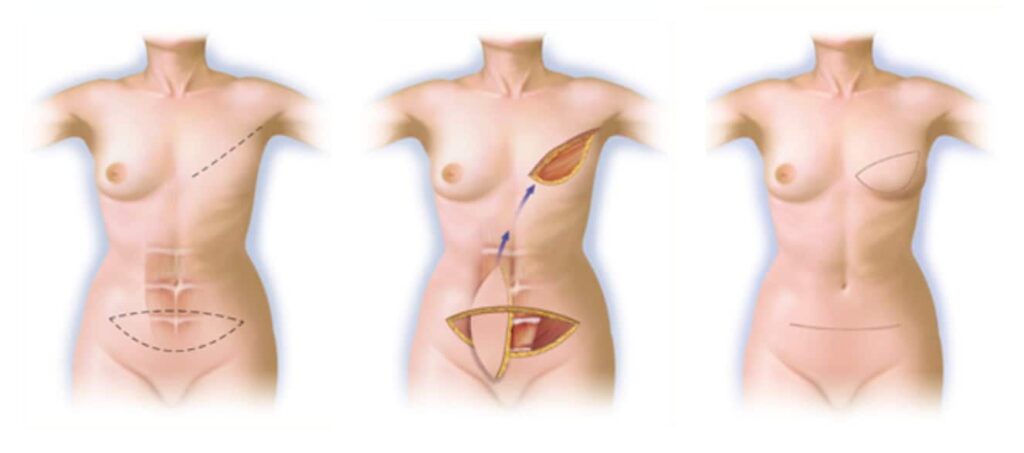
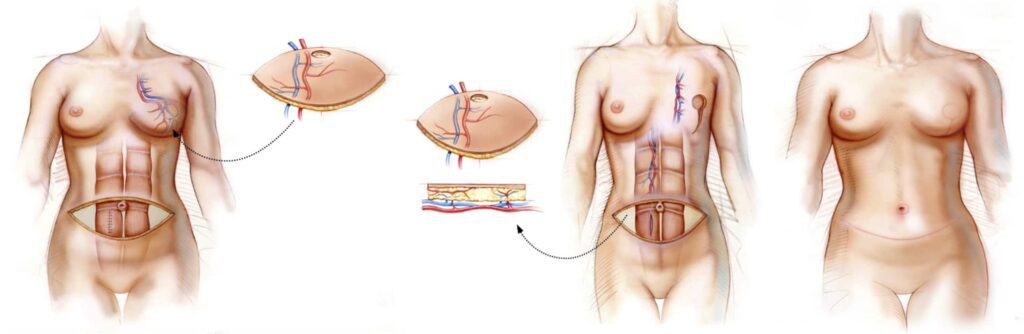
A football shaped piece of abdominal skin and subcutaneous tissue is elevated, same tissue that is used for the DIEP flap, and shaped to recreate a breast mound. This tissue is kept attached to the underlying rectus abdominis muscle, which contains its blood supply (or “pedicle”), and tunneled through the mastectomy site.
Prosthetic Implant with Acellular Dermal Matrix Breast Reconstruction
Traditionally the prosthetic implant breast reconstruction a balloon tissue expander is inserted into the mastectomy site under the pectoralis muscle to create a pocket where the implant will ultimately lie, and then expanded weekly over 2 -3 month period prior to exchanging it for a permanent saline or silicone implant. Acellular dermal matrix is used to create either an “instant pocket” by using the tissue at the lower aspect of the breast acting as a sling or hammock for the implant, or more recent innovation placing the implant over the muscle as a natural breast and creating a pocket covering the entire implant or expander with the tissue avoiding the need to release and cut the muscle. The newer pre-pectoral technique has dramatically decreased the recovery time and recuperation associated with implant based reconstruction and option will be discussed at your consultation. Depending on the size and shape of your breast you may be a candidate to have the permanent implant placed at the time of your mastectomy, either above or below the muscle, sometimes referred to as a direct to implant procedure. This will be discussed at the time of your in office consultation.
If an expander is placed it will be expanded in the office weekly by injection of air into the expander, which is performed weekly at the doctor’s office. After weeks of expansion (usually 6 – 10 weeks), when the pocket is deemed large enough, the patient is taken back to the operating room approximately 4 weeks later to replace the expander with a permanent implant, which may be made of either saline or silicone.
“Dr Farkas and his entire staff were amazing during before and after my surgery. I was comfortable as he answered any questions I had honestly and guided me through the process. My recovery has been easy and my healing is great and I am so happy with my results! I would highly recommend him to anyone considering surgery.”
